How a defibrillator works
Most people think defibrillators are a device that only medical people can use. No doubt you have seen one of those movies where a doctor yells, “Clear!”, and a large shock is administered to a patient, jolting them into the air.
Well we have some good news for you, although these devices are still used by medical teams in hospitals, these are not the defibrillators we use in a public setting.
Thankfully, defibrillators have come a long way and now have been developed into a lightweight, affordable and portable device that can be used by trained and untrained people in a public setting. They are now more commonly called Automated External Defibrillators or AEDs.
A lot of you are still in the dark and don’t know how they work or what they do, so we have put together all the details on what a defibrillator does and how they work, and even more importantly – how safe they are to use!
Firstly, to understand how a defibrillator works, you need to know what happens to someone when they go into cardiac arrest.
Most of us have a normally functioning heart, this means our heart is in sinus rhythm and is functioning normally, the heart’s function is to pump blood around our body and keep everything perfused or supplied with blood and oxygen.
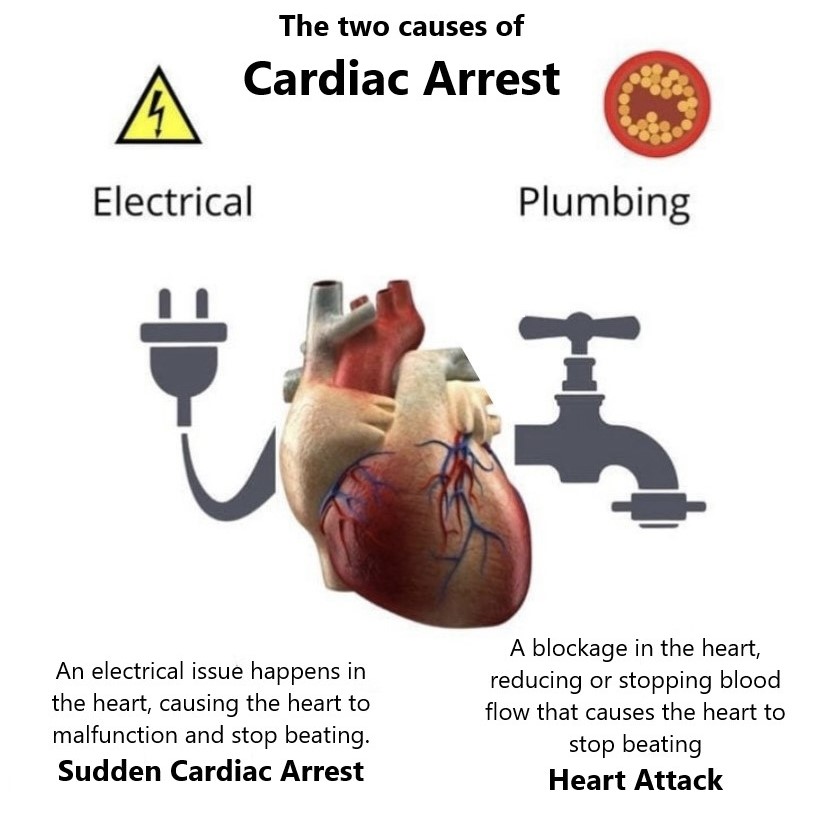
Cardiac arrest happens to someone when their heart stops working properly, this can be caused by a range of things but basically, there are two main causes
- Electrical malfunction, where the hearts electrical system has an issue and the heart stops working, this is commonly known as Sudden Cardiac Arrest (SCA)
- Plumbing malfunction, this is caused by a blockage in a blood vessel around the heart. This is commonly known as a Heart Attack.
In both situations, the heart stops beating effectively and goes into a non-effective rhythm called ventricular fibrillation (VF), or Ventricular Tachycardia (VT), both of these heart rhythms, if not treated urgently result in the death of the patient.
When the heart fibrillates, blood is no longer pumped out of the heart causing no output and no longer flows to the brain or the rest of the body, the patient collapses, stops breathing and is unresponsive. There is no blood flow to the vital organs and the brain and heart primarily start to die rapidly. This is where we get the 10 minute window for resuscitation as every minute indicates a 10% death rate in the heart, and so “Time is Heart” and “Time is Brain!”
How a Defibrillator works
A defibrillator is a fault-finding device that will only shock a patient if their heart is faulty and fibrillating in Ventricular Fibrillation or Ventricular Tachycardia.
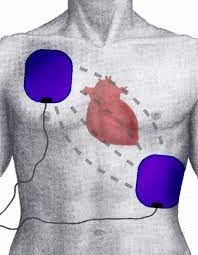
To find a fault, the defibrillator has two pads that are placed onto the patient’s chest in cardiac arrest, the pads are placed either side of the heart and once attached, the defibrillator closes the circuit on the body and goes into an analyse mode, this mode is set to find a fibrillating heart. If the heart is not fibrillating, the device will not shock but if the heart is fibrillating it prompts a shock to be delivered to the patient. The shock passes two electrical currents through the heart, firstly in one direction and then back again, this is called a biphasic shock form or two smaller shocks, this shock depolarises or de-energises the cardiac muscle and stops the heart. The second shock triggers the heart’s electrical impulse or SA node to restart the heart in a normal beating rhythm or sinus rhythm.
What sort of Shock comes out of a Defibrillator?
Automated external defibrillators or AED’s, usually have an in-built escalating energy system and start at a lower electrical shock for a smaller person, then after the first shock, the defibrillator escalates in energy to see if it can be more effective on the second and third shock. The energy output on defibrillators is measured in joules and most defibrillators have set joules for the first, second and third shocks.
These shock protocols will be different for each different defibrillator as the information and success of the defibrillator shock protocol is based on the manufacturer of the defibrillator and the testing and assurance of the device for medical approval – TGA or FDA approval.
The general shock output on a Defibrillator is usually set at the following:
- 1st shock – 100 to 150 joules
- 2nd shock 150 to 250 to joules
- 3rd shock up to 360 joules.
The medical measurement for defibrillation of a patient heart is usually 4 joules of electricity per kilogram of body weight, so higher joule devices are somewhat recommended for a larger patient.
Each different manufacturer of defibrillators around the world also have a card up their sleeve here- they say that the way the defibrillator shocks through the heart can make a difference as well – (the biphasic wave form).
Defibrillators are safe
So, let’s get back to the basics here, remember an AED will not administer a shock unless ventricular fibrillation or ventricular tachycardia is detected in the patient, this is why the defibrillator is safe to use and the rescuer cannot shock a patient unless their heart is faulting.
Now lets look at when to use the Defibrillator.
We recommend following the chain of survival when using a defibrillator in Australia.
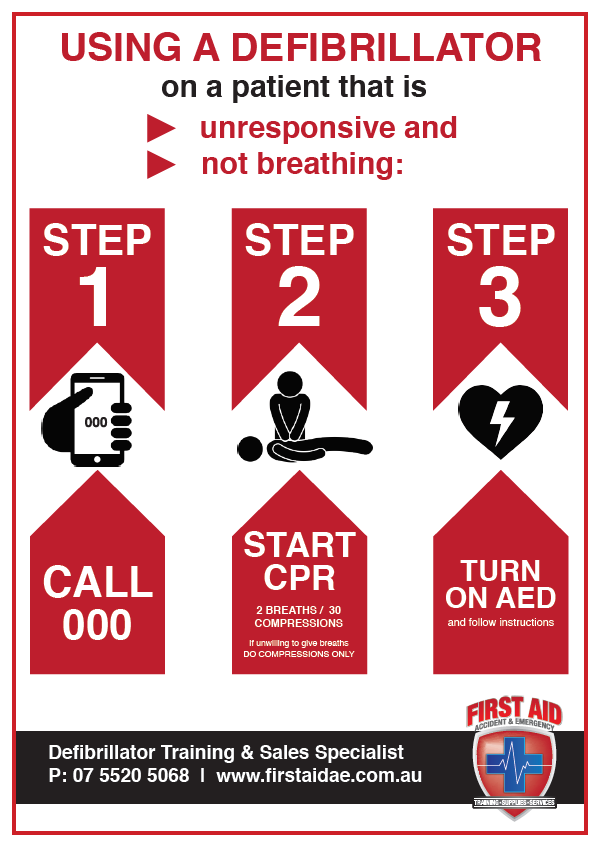
- Early recognition that the patient is in cardiac arrest, this is done by checking the patient’s response, airway and breathing, if the patient is unresponsive, and not breathing make an early call to 000 immediately.
- Start CPR on the patient, CPR is aimed at manually pushing the blood around the body to prevent brain and heart damage.
- Turn on the defibrillator and follow the prompts. The defibrillator will give voice prompts and ask the responder to call emergency services and then ask the responder to expose the patient’s chest. Once this is done the defibrillator will prompt the rescuer to peel the electrode pads off the plastic and place them on the patient’s chest as shown on the pad diagrams. Typically, one electrode is placed just below the patient’s right clavicle, while the other is placed just below and to the left of the pectoral muscle on their left-hand side. This position allows for an effective current for both ECG readings and defibrillation. We call this the Driver’s seat belt position.
- The Defibrillator will ask the responder to cease CPR momentarily and the AED will analyse the patient’s heart rhythm. If the rhythm indicates that defibrillation can help, the machine will either instruct you to press the shock button or to step back from the electrodes as it administers the shock automatically. Make sure nobody touches the patient at this time.
- When the AED indicates that it is safe to do so, continue with CPR until the patient shows signs of restored heart function or help arrives. The AED may instruct you to administer additional shocks.
- If the AED indicates that the patient does not display a shockable rhythm, continue with CPR until the patient starts breathing or emergency services arrive.
CPR prevents Brain Damage – “Time is Brain”
Remember – CPR is just as important as defibrillation in the event of sudden cardiac arrest. Chest compressions can help manually pump blood to deliver oxygen rich blood to the brain. CPR helps delay tissue death in the brain and heart until defibrillation begins!
So make sure you learn how to do CPR
It is also important that a defibrillator does not restart a heart that is in Asystole or has stopped. The patient in cardiac arrest usually has a fibrillating heart for approximately 10 minutes, after the 10 minute window the patient will proceed into flat line or Asystole, the defibrillator will not work on flat line and the chance of survival is now as low as 1%.
Therefore it’s so important to get a defibrillator on a patient in the first 10 minutes of a cardiac arrest to try and rectify the faulting heart.
Ultimately, if we can recognise a patient in this state, perform good quality CPR and defibrillate the patient, we can increase survival to 75% and in doing so – save more lives!
Check out our Defibrillator packages here: Medical Shop.